
We’ve designed this page to help you learn about dementia in clear, compassionate language. You may be:
- Navigating a recent diagnosis
- Concerned about a loved one
- Simply trying to understand what dementia means
Whatever led you here, this guide will have something for you. We’ll explain what dementia is, what causes it, how it progresses, and what care options are available.
You’ll also find helpful links to more in-depth articles and resources. Wherever you are on your journey with dementia, we hope this guide brings you clarity and comfort. You can always visit the EPOCH Exchange, our hub for further memory care resources, including insights, caregiver tips, podcasts, and more.
If you’re exploring care options, view our guide to memory care communities.
What Is Dementia?
Dementia is a general term for a decline in memory, language, and thinking that affects daily life. Dementia isn’t one specific disease. Instead, it refers to a group of symptoms caused by changes in the brain. Much like “heart disease” describes several heart-related conditions, dementia is an umbrella term for many different types of memory loss.
Alzheimer’s disease is the most common form of dementia, accounting for 60-80% of all cases. Others include vascular dementia, Lewy body dementia, and frontotemporal dementia. We’ll cover each in more detail later.
Alzheimer’s is a progressive brain condition. It slowly damages brain cells, leading to memory loss, confusion, and difficulty with daily tasks.
Although it becomes more common with age, Alzheimer’s is not a normal part of growing older. It develops over time and gradually worsens. While research is ongoing, there is currently no cure for Alzheimer’s.
What Are the Symptoms of Dementia?
Dementia affects everyone a little differently. Memory loss is the symptom often most associated with dementia and the one people recognize the most, but there are others.
Dementia can also affect how a person thinks, communicates, moves, and interacts with others. Some symptoms are more prevalent than others, depending on the form of dementia.
Some of the more common symptoms include:
- Trouble remembering recent events or conversations
- Difficulty finding the right words
- Trouble following conversations
- Confusion about time, places, or familiar routines
- Struggling with planning and problem-solving
- Trouble making decisions
- Changes in mood, personality, or behavior
- Aggression
- Anxiety/depression
- Restlessness/wandering
- Sundowning
- Withdrawal from hobbies or social activities
- Trouble handling money or managing medications
- Repeating questions or forgetting appointments
- Poor judgment or safety awareness
- Balance issues
- Hallucinations
Summary of symptoms in four categories:
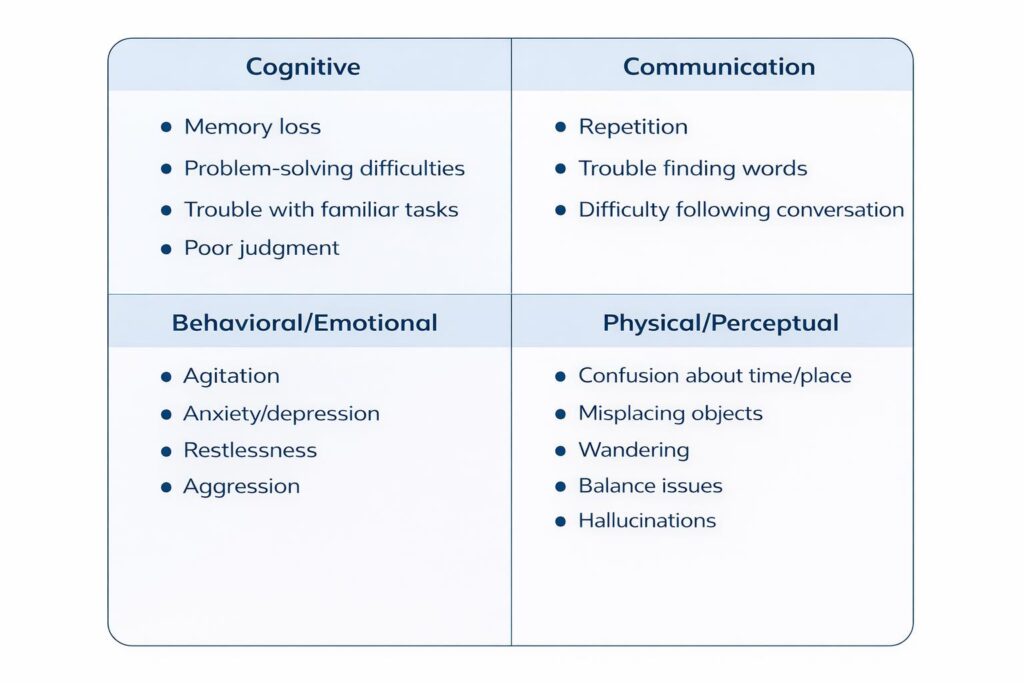
Read more about these symptoms in our blog that highlights the 10 early warning signs of dementia.
If someone you care about is showing one or more of these signs, or even just seems different in ways you can’t explain, it’s a good idea to check in with a medical professional.
“Many health issues can look like dementia but are actually treatable. For example, difficulty following conversations or withdrawal from social activities could be related to a hearing issue, or a UTI can cause temporary troubling symptoms similar to those of dementia.”
Alicia Seaver, Vice President of Memory Care Operations
Getting answers early helps rule out other causes and, if it is dementia, allows for better planning, care, and support for the road ahead.
While there’s no cure yet, early detection of dementia can make a real difference in quality of life for everybody involved.
What Causes Dementia?
Dementia starts when brain cells get damaged. This damage disrupts how cells send and receive messages. This, in turn, affects memory, judgment, and behavior.
Alzheimer’s disease causes most cases of dementia. In this condition, abnormal proteins build up in the brain, interfering with the proper functioning of cells. Other types of dementia have different causes, such as changes in blood flow or the presence of unusual proteins.
Medical conditions can also lead to symptoms that look like dementia. Some of these may improve with treatment, so it’s important to talk with a doctor if something seems off.
Conditions That Typically Progress Over Time
These illnesses gradually worsen and do not have a cure at this time:
- Alzheimer’s disease
- Vascular dementia (linked to stroke or blood flow problems)
- Lewy body dementia
- Frontotemporal dementia
- Mixed dementia (a combination of more than one type)
- LATE (a condition that affects older adults with changes in a specific brain protein)
Other Possible Causes and Contributing Factors
These conditions may cause similar symptoms or increase the risk of dementia:
- Normal pressure hydrocephalus
- Creutzfeldt-Jakob disease
- Huntington’s disease
- Chronic traumatic encephalopathy (CTE)
- HIV-associated dementia
- Traumatic brain injury
- Long-term alcohol use
- Side effects of medications
- Thyroid disorders
- Low vitamin B12 or other deficiencies
- Delirium caused by illness or infection
- Depression, anxiety, or extreme stress
Here’s a summary table:
| Cause | Description | Progressive or Treatable |
| Alzheimer’s Disease | The most common cause of dementia. Affects memory, thinking, and behavior. | Progressive |
| Vascular Dementia | Caused by reduced blood flow to the brain, often after a stroke. | Progressive |
| Lewy Body Dementia | Caused by abnormal protein deposits (Lewy bodies) in the brain. | Progressive |
| Frontotemporal Dementia | Affects the frontal and temporal lobes of the brain, often leading to behavior and language changes. | Progressive |
| Mixed Dementia | A combination of two or more types of dementia, often Alzheimer’s and vascular dementia. | Progressive |
| LATE (Limbic-predominant Age-related TDP-43 Encephalopathy) | A newer identified condition that mimics Alzheimer’s symptoms. | Progressive |
| Huntington’s Disease | A genetic disorder causing degeneration of brain cells. | Progressive |
| Creutzfeldt-Jakob Disease | A rare, rapidly progressing brain disorder caused by prion proteins. | Progressive |
| Chronic Traumatic Encephalopathy (CTE) | Caused by repeated head injuries, commonly seen in athletes. | Progressive |
| Normal Pressure Hydrocephalus (NPH) | A buildup of cerebrospinal fluid in the brain’s ventricles. | Sometimes Treatable with Surgery |
| HIV-associated Dementia | Occurs in later stages of HIV/AIDS due to brain damage caused by the virus. | Sometimes Treatable |
| Medication Side Effects | Some medications can cause memory issues or confusion. | Often Reversible |
| Depression and Anxiety | Can mimic dementia symptoms in older adults. | Treatable |
| Thyroid Problems | Both hyperthyroidism and hypothyroidism can lead to cognitive issues. | Treatable |
| Vitamin Deficiencies (e.g., B12) | Lack of certain vitamins can affect brain health. | Treatable |
| Delirium | A sudden change in mental status caused by illness or medication. | Reversible |
| Head Trauma | A serious blow to the head can lead to memory problems. | Varies by Severity |
| Heavy Alcohol Use | Long-term alcohol abuse can damage brain cells. | May Improve with Sobriety |
Since we can treat some of these conditions, early evaluation and monitoring often make a difference. If you notice changes in someone’s memory or behavior, speaking with a medical professional is a good place to start.
Note: You’ll notice this is a general theme across all of our advice: speak up and seek help if you have any concerns. It bears repeating, since it’s critical to seek help early.
If you want to learn more about dementia and caregiving, we host regular education sessions and offer caregiver support groups, both in-person at our communities and virtually.

Take a look at our upcoming event schedule:
What Are the Stages of Dementia?
When we say that dementia progresses over time, we mean the symptoms worsen. While the exact experience and rate of change varies for each person, many experts describe the condition in ‘stages’ that help us track the disease.
These stages can help individuals and families understand what changes to expect and when more support may be needed. You’ll hear caregivers and medical professionals talking about an individual’s baseline. Professionals want to track whether there are changes to this baseline on a day-to-day basis. This ‘baseline’ essentially means where the person with dementia is at (referring to their symptoms) at any given moment.
“Understanding an individual’s baseline essentially helps to ‘place’ an individual in a certain stage.”
Alicia Seaver, Vice President of Memory Care Operations
Before the first official stage of dementia, many people experience a phase known as Mild Cognitive Impairment, or MCI.
Mild Cognitive Impairment (MCI)
MCI is a noticeable decline in memory or thinking skills that’s more than normal aging, but not severe enough to interfere with daily life. It is often a precursor to dementia. Symptoms include:
- Forgetting recent events or appointments
- Struggling with decision-making
- Difficulty focusing or following conversations
Not everyone with MCI develops dementia, but it can be an early warning sign, especially if memory issues begin to affect confidence or routine.
Early Stage (Mild Dementia)
Symptoms may be subtle and easy to dismiss as aging.
- Misplacing items or forgetting names
- Difficulty with planning or complex tasks
- Feeling overwhelmed in new or busy environments
- Increased anxiety or irritability
People at this stage usually remain independent but may benefit from structure and gentle support to counterbalance these symptoms.
Middle Stage (Moderate Dementia)
This is typically the longest stage and includes more pronounced symptoms.
- Forgetting familiar people, places, or routines
- Needing help with dressing, cooking, or managing medications
- Changes in mood or behavior, such as confusion or agitation
- General resistance or refusal to cooperate
- Repeating questions
- Wandering
- Rummaging or hoarding
Supervision becomes increasingly important as caregivers deal with greater responsibilities. At this stage, many families begin exploring professional memory care options (but we think many would benefit from memory care in earlier stages).
Late Stage (Severe Dementia)
At this point, dementia significantly affects both physical and cognitive abilities, making activities of daily life almost impossible to do alone.
- Minimal verbal communication
- Difficulty eating or swallowing
- Needing full assistance with all personal care
- Sleeping more and withdrawing from surroundings
Comfort, dignity, and emotional connection are the focus of care in this stage.
Learn more about the types and stages of dementia

What Leads to a Dementia Diagnosis?
“Diagnosing dementia is not about one single test. It involves a careful review of a person’s symptoms, medical history, and behavior. The goal is to determine whether memory loss or confusion is part of normal aging or something more serious.”
Alicia Seaver, Vice President of Memory Care Operations
Who Makes the Diagnosis?
A diagnosis may start with a primary care doctor, but specialists like neurologists, geriatricians, or psychiatrists can also get involved. These professionals have the training to recognize the signs of dementia and rule out other causes. We can often think about a dementia diagnosis as a process of elimination, as professionals look for other causes of memory loss first.
How Is Dementia Diagnosed?
Doctors use several tools to make a diagnosis:
Cognitive tests
These are short tasks that check memory, problem-solving, and attention. One common tool is the Mini-Mental State Examination (MMSE). There is a self-administered Alzheimer’s test that you can take.
Neurological exams
These check for balance, reflexes, and other signs of brain function.
Brain imaging
Scans like an MRI or CT can show signs of stroke, tumors, or shrinkage in certain brain areas. These findings help doctors rule out other causes and spot changes linked to dementia.
Psychiatric evaluation
This step helps doctors separate dementia from depression, anxiety, or other mental health issues that can affect memory.
Lab work
Blood tests can find problems like vitamin deficiencies or thyroid issues. These conditions can mimic dementia and may be treatable.
Spinal fluid tests
In some cases, doctors use cerebrospinal fluid (CSF) analysis to look for changes linked to Alzheimer’s or other types of dementia.
Genetic testing
While not routine, this may be recommended if there’s a strong family history of dementia or if symptoms appear early in life.
Why Does Early Diagnosis Matter?
“The sooner we can diagnose dementia, the more time families have to plan. Early diagnosis gives people a chance to make decisions about care, finances, and legal matters while they can still be involved. An early diagnosis also opens the door to new therapies or clinical trials that may be most effective in the early stages.”
Alicia Seaver, Vice President of Memory Care Operations
We sat down with Camille Ciarametaro, Senior Advisor at Bridges by EPOCH of Lexington, to discuss the benefits of detecting dementia early. Camille explores how an early diagnosis is beneficial for everybody involved:
What Are the Dementia Treatment and Care Options?
There is currently no cure for dementia, but a combination of treatments can help manage symptoms and improve quality of life. Each person’s needs will vary, and the most effective care plan often involves a mix of medical, emotional, and environmental support.
Medications
Several medications can help reduce symptoms or slow the progression of some types of dementia, especially in the early stages.
- Cholinesterase inhibitors (like donepezil, rivastigmine, and galantamine) may improve communication between brain cells and help with memory, judgment, and thinking.
- Memantine works by regulating a chemical involved in learning and memory. It’s often used for moderate Alzheimer’s.
- Doctors may also prescribe medications to treat related symptoms such as depression, anxiety, sleep issues, or aggression.
Medication doesn’t stop dementia, but it can provide relief and improve functioning for a period of time.
Non-Medical Therapies
Non-drug therapies play an important role in care. These approaches focus on preserving abilities, reducing stress, and enhancing well-being.
- Occupational therapy helps individuals adapt their living spaces and routines to stay as independent as possible.
- Cognitive stimulation includes memory games, puzzles, technology, and conversation-based activities that engage the brain.
- Music and art therapy can reduce anxiety, spark memories, and offer meaningful self-expression at all stages of dementia.
- Routine and structure create predictability and comfort, especially for those who struggle with changes or unfamiliar environments.
- Aromatherapy and touch are vital to soothe those experiencing agitation. Calming scents and gentle hand massages can work wonders as part of a broader non-pharmacological care program.
For many people, medication can turn down the volume to allow non-medical strategies to lead to the best outcomes. We should always try to satisfy the individual’s needs first (are they hungry, tired, in pain?) before we resort to medications.
In a recent podcast episode, we spoke with Rosemary Ombewa, Wellness Director at Bridges Andover, about non-pharmacological approaches to dementia care.
What Is Memory Care Assisted Living?
“When someone reaches the point where they need more daily support and supervision, memory care assisted living may be the right fit. We think it can benefit residents to enter memory care even before they need this level of support.”
Alicia Seaver, Vice President of Memory Care Operations
These specialized communities are designed to meet the needs of individuals living with Alzheimer’s or other forms of dementia.
Memory care communities offer:
- A secure, purposefully designed environment to help residents thrive
- Structured daily routines
- Specialized programming that supports memory, independence, and dignity
- Team members trained in dementia care
- Assistance with daily living, such as bathing, meals, and medication
- Supportive technologies to improve quality of care and quality of life
You can read more in-depth about what memory care involves in our What Is Memory Care? resource.
How Bridges® by EPOCH Can Help
At Bridges® by EPOCH, we’ve designed purposefully built communities for individuals living with memory loss. We focus on compassionate, person-centered care delivered by professionals who understand the unique needs of those with dementia.
Residents benefit from daily engagement, sensory therapies, and opportunities for social connection, all designed to meet them where they are in their journey.
We know how challenging this decision can be. Whether you’re ready to take the next step or just starting to explore options, we’re here to help.

Find a community near you using our locator:
What Are Dementia Risk Factors?
Some factors that increase the risk of dementia cannot be changed, while others we can influence through things like lifestyle or medical care. Understanding all these risk factors can help with prevention and early planning.
Risk Factors You Can’t Change
- Age
The risk of dementia increases as people get older. Most cases occur in individuals aged 65+. - Family History and Genetics
People with a parent or sibling who had dementia may be more likely to develop it themselves. Certain genes, such as APOE-e4, are linked to higher risk, especially in Alzheimer’s disease.
Risk Factors You May Be Able to Change
There are many areas of your health and lifestyle where small changes may help protect your brain.
“In recent years, research has shown a strong connection between overall wellness and reduced risk of cognitive decline. Addressing these risk factors (living more healthily, basically) won’t guarantee prevention, but it may help delay the onset or lessen the severity of symptoms.”
Alicia Seaver, Vice President of Memory Care Operations
Here are the areas experts believe are most important
Cardiovascular Health
Conditions like high blood pressure, high cholesterol, diabetes, and heart disease are linked to greater dementia risk.
What helps: Managing blood pressure, maintaining healthy blood sugar levels, and keeping cholesterol in check can support both heart and brain health. Go for regular check-ups to check on your heart health to stay on top of these risk factors.
Physical Inactivity
A sedentary lifestyle can contribute to poor brain and heart health.
What helps: Aim for regular exercise to stay fit, but you don’t need to go overboard. A little light exercise goes a long way. Walking, swimming, gardening, or group fitness classes can all help increase circulation and keep the brain active. The main lesson here is that a lack of movement is going to cause all sorts of harm to your body.
Poor Diet
Diets high in processed foods and saturated fats may raise dementia risk.
What helps: A Mediterranean-style diet, rich in vegetables, whole grains, healthy fats, and lean proteins, may help protect cognitive health. Eating chips, sweets, soda, and fried foods regularly is likely to increase your dementia risk.
Smoking and Alcohol Use
Both habits are associated with a higher risk of dementia.
What helps: Quitting smoking and reducing alcohol intake improve brain function and support overall wellness. If this feels difficult, ask your doctor about available support programs.
Hearing and Vision Loss
Untreated sensory loss can contribute to social withdrawal and reduced brain stimulation.
What helps: Get regular hearing and eye exams and use hearing aids or glasses when needed. These adaptations can help you stay engaged and connected. The key underlying purpose here is to remain socially engaged, which is so important to ensure brain stimulation.
Depression and Anxiety
Mental health issues can affect memory, focus, and daily function.
What helps: Talk therapy, medication, and mindfulness practices can make a difference. Prioritizing emotional well-being may also help protect cognitive function long-term.
Sleep Disorders
Chronic sleep problems, like insomnia or sleep apnea, can harm your ability to concentrate while also making you less likely to be able to recall things.
What helps: Practicing good sleep hygiene and seeking treatment for conditions like apnea may improve sleep quality and cognitive clarity.
Air Pollution
Long-term exposure to air pollution has been linked to higher dementia risk in some studies.
What helps: While harder to control, using air purifiers indoors and limiting time outdoors on high-pollution days may help reduce exposure. This is reminiscent of the rise of dementia cases associated with lead poisoning decades ago, before lead was removed from gas.
Vitamin Deficiencies
Low levels of B vitamins, vitamin D, and other nutrients may impact brain health.
What helps: A well-balanced diet and regular blood tests can identify and address deficiencies. A doctor might recommend supplements if you exhibit particularly low levels.
What Is the Role of Cognitive Reserve and Lifelong Learning?
In recent years, researchers have explored why some individuals show fewer symptoms of dementia despite having physical signs of brain disease. One explanation is cognitive reserve, which is the brain’s ability to adapt and use alternate pathways to compensate for damage.
People who engage in mentally stimulating activities throughout life, such as reading, learning new skills, working in intellectually demanding jobs, or even staying socially active, may develop stronger and more flexible neural connections.
These connections can help the brain “work around” or “persevere” through damage for a longer period of time.
“Some studies suggest that individuals with a higher IQ and lifelong learners may be at a reduced risk of developing dementia. Their brains may not necessarily avoid the disease, but they may be more resilient in coping with its effects. This resilience is part of what scientists mean when they refer to ‘cognitive reserve’.”
Alicia Seaver, Vice President of Memory Care Operations
Ways to build or maintain cognitive reserve include:
- Reading books, newspapers, or educational content
- Playing strategy games or puzzles
- Learning new hobbies, languages, or instruments
- Engaging in meaningful social interactions
- Staying physically active (which also supports brain health)
Remember that It’s never too late to begin. Even in later life, adding new forms of mental stimulation and keeping the brain active can offer protective benefits.
Living with Dementia
Dementia affects more than memory. It reshapes daily life, changes relationships, and places new demands on everyone involved.
While clinical information explains what dementia is, it cannot fully capture how it feels to live with it. Knowing what it is also doesn’t provide a neat blueprint for care, either.
This section explores what dementia looks like beyond the diagnosis. It gives a fuller picture of the experience for both individuals and their families.
What Is it Like Inside the Mind of Someone Living with Dementia?
When dementia begins to affect the brain, everyday tasks may feel confusing or overwhelming. A person might struggle to make sense of their surroundings. They may withdraw or respond with frustration when something feels unfamiliar.
This confusion does not mean the person is lost to us. People with dementia often respond to music, gentle prompts, or a familiar face, even if they can’t express recognition clearly. Simple pleasures, such as a favorite song or a quiet walk, may still bring comfort.
They are still present, even if the way they communicate has changed. It just takes a different approach to connect.

How Does Dementia Change Relationships?
As dementia progresses, the nature of a relationship can shift. A spouse may take on more responsibilities. A child may start making decisions for a parent, and it can be hard to negotiate family dynamics. Friends may notice fewer shared conversations or moments of connection.
These changes bring grief. For many caregivers, it feels like they are slowly losing someone they love. This grief can feel complicated because the person is still physically there.
It helps to understand that relationships do not disappear. They become something new. The emotional connection remains, although it may take different forms. A shared smile, a gentle touch, or a familiar phrase can still mean a great deal.
How Can We Support Caregivers?
Caring for someone with dementia can be overwhelming. Many caregivers feel uncertain. They are often unsure how to communicate or respond to sudden changes in behavior.
Support makes a difference. Caregivers benefit when they learn ways to adjust to the person’s needs. For example, simplifying tasks, using visual cues, or finding a calming routine can ease daily interactions. These approaches require patience, but they help maintain connection and reduce frustration for both people.
When caregivers feel supported, they are more confident and more emotionally resilient. This helps them continue their role with strength and clarity.

Here’s a selection of articles from the EPOCH Exchange on caregiver advice:
- It’s okay to ask for help
- Effective communication tips
- Dementia caregiving tips and tricks
We also offer plenty of support for caregivers each month through educational sessions and support groups, with both in-person and virtual events available:
Take a look at our upcoming event schedule:

And, finally, we also offer plenty of advice via our monthly podcasts that cover various topics related to dementia care and senior living more broadly. Here’s our episode on reducing caregiver stress, with expert insights from Amy Murray, Executive Director at Bridges by EPOCH at Andover.
A Shared Experience: What Is the Dyad of Care?
The dyad of care is a model of care that treats the patient and their family as one single unit. When we think of care provision, we need to think of everybody affected by any given disease.
In dementia care, the idea of the dyad of care means the caregiver becomes part of the process, acknowledging they need treatment and guidance, too. It is also a recognition that the caregiver’s health and emotional well-being directly affect the quality of care their loved one receives.
Despite this, caregivers often receive little support. They are expected to manage daily routines, emotional decisions, and long-term planning, all while carrying the weight of uncertainty.
Support systems are essential. At Bridges®, we work to make sure caregivers are not alone. We provide:
- Information that fits each stage of the journey.
- Training in safe and effective care techniques.
- Space to express emotions and find community through support groups.
We believe that caring for the caregiver is not optional. It is part of the care plan.
How Do We See the Person Beyond the Diagnosis?
Sometimes, dementia becomes the main focus. But we must not lose sight of the individual behind the condition.
Meaningful moments still happen. A person may light up at a song they love or become calm when looking at family photos. These reactions show that their identity is still present.
Caregivers often say that these moments remind them of who their loved one is. Small connections bring joy and meaning. The goal is not to fix the disease but to find the person within it.

