Table of Contents

Dementia changes the rhythm of your marriage as care tasks can take over days. Your relationship will change, but the love you share still matters. You can protect that loving relationship with some clear habits and support when you need it.
What Should You Keep in Mind as Dementia Progresses?
Dementia changes over time, and early-stage needs often look different from later-stage needs. You may still plan and decide together, navigating the changes together for now. The harder truth is you still need to prepare for higher care needs later.
If you want a comprehensive overview, head to our guide to dementia, and supplement that with our guide to memory care.
Wherever you are on your journey, it’s helpful to think of two tracks:
- Live well together today with routines and connection
- Plan ahead for safety, support, and future care choices
What Changes When Your Partner Has Dementia?
Your roles can shift from partners to caregiver and care receiver. You may manage the home, the schedule, and the decisions; responsibilities you likely shared before. You may also be juggling a career, too.
Your partner may act in ways that feel out of character, and you may be afraid of the changes to come. See this overview of potential behaviors:
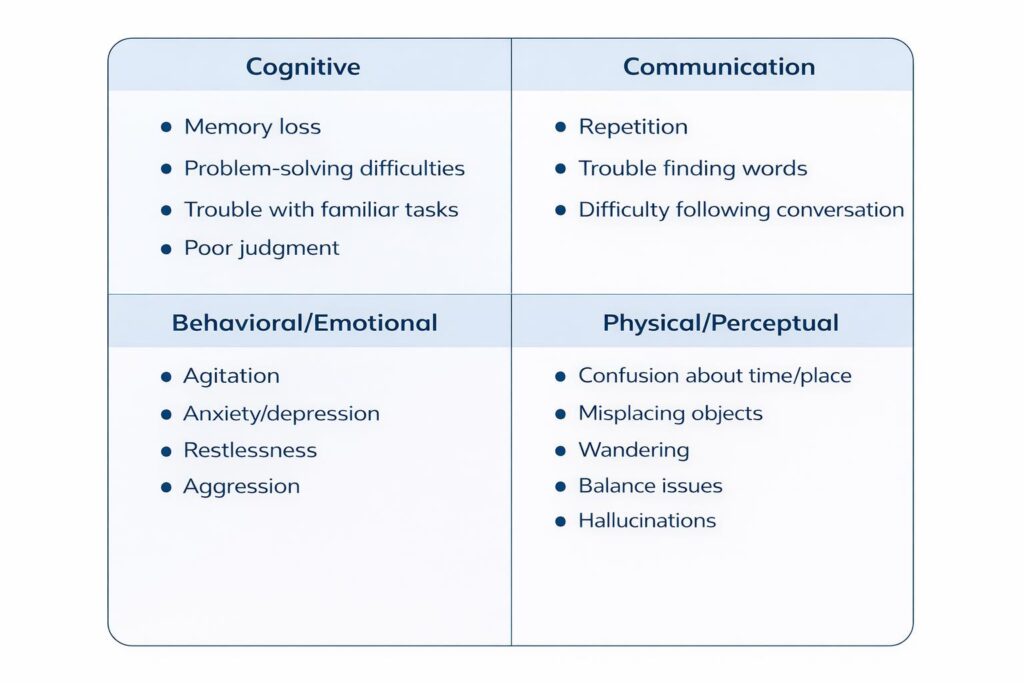
All this results in what can be an extremely challenging and emotional dynamic. You may face:
- High stress
- Less social time
- Depression or anxiety
- Financial strain
- Less time for your own health
- Less sleep
How Do You Reset Expectations as a Couple?
For as long as you can do so, you set new expectations for what “normal” looks like. You also name what you can still do together.
Start with three decisions:
- What must happen each day for safety
- What support you need each week
- What you will protect for your relationship
This last one is important. It’s how you commit to remaining partners in the face of those changing dynamics due to the symptoms of dementia. Try a question like this: “What can we do this week that feels like us?”
How Can You Be Both a Caregiver and a Partner?
Extending this idea, you must schedule “couple time” on purpose. Keep it simple and something you can repeat.
For example, choose a daily habit:
- Share a coffee together
- Take a short walk
- Listen to favorite songs together
- Read aloud for ten minutes together
- Look at photos to reminisce
These are general, low-barrier-to-entry things to do together. You can probably come up with other activities specific to your hobbies, preferences, and abilities. The point is you mark these moments as essential. Even write them on a calendar if you need to keep yourselves accountable.
What Do You Do when Behaviors Feel Personal?
Dementia can change mood, judgment, and impulse control. Your spouse may accuse you or lash out.
These moments can be troubling and upsetting. It is important to try and remember that your partner isn’t purposefully doing these things; they are symptoms of the disease. You can only control how you respond.
So, strive to respond in ways that lower stress and agitation.
Use a short, steady script:
- “I hear you.”
- “You feel upset.”
- “I’m here with you.”
- “Let’s take a break.”
These phrases validate your partner’s feelings – a critical step in compassionate dementia care.
Then redirect:
- Offer a drink or snack
- Move to a quieter room
- Start a calming activity
You don’t need to argue facts. This approach is likely, in fact, to further inflame the situation. Your priority is to reduce agitation as you need to keep the moment safe.
How Do You Keep Your Partner Involved in Decisions?
Dementia care is often about preserving dignity for the individual experiencing memory loss. Allowing agency while keeping them safe is key. So, offering two safe options is always a good tactic.
Examples:
- “Would you like tea or water?”
- “Shall we go for a walk now or after lunch?”
- “Are you going to wear the blue shirt or gray shirt?”
This approach reduces conflict while supporting independence. The opposite, merely ‘telling’ your spouse or partner what to do, when to eat, how to dress, etc., is belittling and will likely lead to resentment.
How Do You Protect Your Health as a Caregiver?
You need stamina for this role. You protect your spouse when you protect your basics. Use these quick checkpoints and adjust them as needs change.
Protecting Your Health
Are you sleeping enough?
Lack of sleep makes everything harder and raises your risk of burnout.
– Set a firm bedtime when you can
– Ask someone to cover one evening a week
– Tell the doctor if sleep problems last more than two weeks
Are you eating real meals?
Skipped meals lead to low energy and short patience.
– Keep easy basics on hand (yogurt, soup, eggs, fruit)
– Set three meal “anchors” in your day
– Accept meal drop-offs or a meal service if needed
Are you moving your body most days?
Movement lowers stress and supports sleep.
– Take a 10–20 minute walk
– Stretch while the kettle boils
– Use one short routine you can repeat daily
Are you keeping your own medical appointments?
Caregiving often pushes your health to the bottom, but you must see your health as a priority.
– Schedule your next visit before you leave the office (or when you have a free moment)
– Write down symptoms and questions
– Ask a friend to cover care during appointments
Do you have at least one support touchpoint each week?
Isolation builds fast, which is damaging in itself. Reaching out for support offers an opportunity to socialize while also potentially receiving help and advice.
– Call one person who listens well
– Join a caregiver support group
– Talk with a counselor if stress stays high
Are you seeing signs of burnout?
Burnout shows up in your body and mood. Treat it as a signal that you need to do something about it. Certainly, don’t treat it as a failure.
Look for:
– Constant exhaustion
– Irritability or numbness
– Frequent headaches or stomach issues
– Losing interest in things you used to enjoy
If you see these signs, ask for help now. Call your doctor or a local caregiver resource line.

Take a look at our upcoming caregiver support groups
When Should You Ask for Help and Respite Care?
So, even if you do take care of yourself, you are still likely to need help in some form at some point as the disease progresses, whether you need a break or you simply can’t cover all your loved one’s needs safely by yourself.
Make a task list that others can help you with:
- Grocery runs
- Meal drop-offs
- Laundry
- Rides to appointments
- Two-hour sitting visits
- Paperwork and phone calls
Also consider:
- Adult day programs
- In-home care
- Respite stays
- Caregiver support groups
When you are feeling overstretched, there is power in small acts of help. Direct requests work best, so don’t be afraid to ask, especially if someone offers their help. Say what you need and when you need it.
A two-hour sitting visit from somebody you trust can be a real help that allows you to recharge and take a moment for yourself.
Our Executive Director at Bridges by EPOCH at Andover, Amy Murray, has spoken eloquently about caregiver stress. Her main message? That it’s okay to ask for help!
While not explicitly about spousal caregivers, you may find this episode of the EPOCH Exchange podcast useful. It explores the signs of caregiver burnout and what you can do to avoid it:
How Do You Handle Intimacy Changes?
Dementia can change desire, comfort, and boundaries. You may also feel tired or unsure. You can still keep closeness in safe ways.
Focus on:
- Hand holding
- Hugs
- A shoulder rub
- Sitting close
If sexual behavior becomes unsafe or unwanted, set clear limits. Ask a clinician for guidance.
Different Situation: How Do You Support a Spousal Caregiver?
Let’s say your partner carries caregiving duties, say for their parent or a sibling. This is likely to be a significant commitment that will change your relationship for the time that they are caregiving.
You can reduce the load fast. You do it with action, not vague offers. You show empathy and understanding, showing you are also part of the caregiving team.
Do these five things:
- Learn the diagnosis and the care plan
- Take household tasks without waiting
- Listen and stay steady
- Protect breaks and boundaries
- Schedule time for your relationship
Use direct offers:
- “I will handle dinner every Tuesday.”
- “I will sit with your parent/sibling Saturday morning.”
- “I will make these calls today.”
Part of this is automatically taking up the baton and showing up for them in ways you know will help.
However, you can also ask them directly: what else do they need from you?
How Do You Stay Present While Planning Ahead?
Dementia changes over time. You need to plan for safety, care, and support to help you avoid rushed decisions later. Yet, planning can also pull you into constant “what if” thinking.
Alongside this planning, you should try to stay present.
Staying present keeps your days from shrinking down to tasks and worry. You don’t ignore the hard parts, but train yourself to notice the good parts that still happen. You look for small moments of joy among the challenges.
Many people feel it is useful to practice gratitude in small ways:
- Write down one good thing that happened each day
- Notice one moment you shared together
- Say one thank you out loud
- End the day with a small gesture of connection
These small actions help you stay grounded while you keep planning for what comes next.
When Is Memory Care the Right Next Step?

Sometimes care needs exceed what you can provide at home. That change can feel hard, but we need to come to terms with the idea that a move can also improve safety and stability.
Watch for these signs:
- Safety risks at home
- Wandering or frequent falls
- Aggression you cannot manage
- Nighttime wake-ups that disrupt sleep
- Missed meals or medications
- Ongoing caregiver exhaustion
Memory care can provide structure, trained support, and a secure space. It can also give you room to be a partner again. Learn more about transitioning to memory care and understanding when it may be the right move.
How Can Bridges® by EPOCH Support You?
Bridges® by EPOCH provides dementia-focused memory care and support for loved ones. We design care for changing needs across all stages of dementia, allowing residents to age in place.
You can expect:
- A secure, purposefully-designed environment for those with dementia
- Dementia-trained team members
- Life enrichment programs that support strengths and routine
- Support groups and educational events
- Care plans that adapt over time
To learn more, continue to explore our resources center for other insights, podcasts, and caregiver tips.
Contact us to learn more or schedule a tour. Fill out the form below, and a team member will be in touch.
